Monitoring the First Year of the COVID-19 Pandemic in New Orleans and Louisiana
Published: Mar 24, 2020
The COVID-19 Pandemic is having an unprecedented impact on New Orleans, Louisiana, the United States and indeed the world. This webpage provides the most up-to-date data on COVID-19 cases and deaths in Louisiana, the metro, New Orleans and other early hot spots across the U.S. Check back often for updated stats and a full archive of historical data since inception.
Tracking COVID-19 in Louisiana
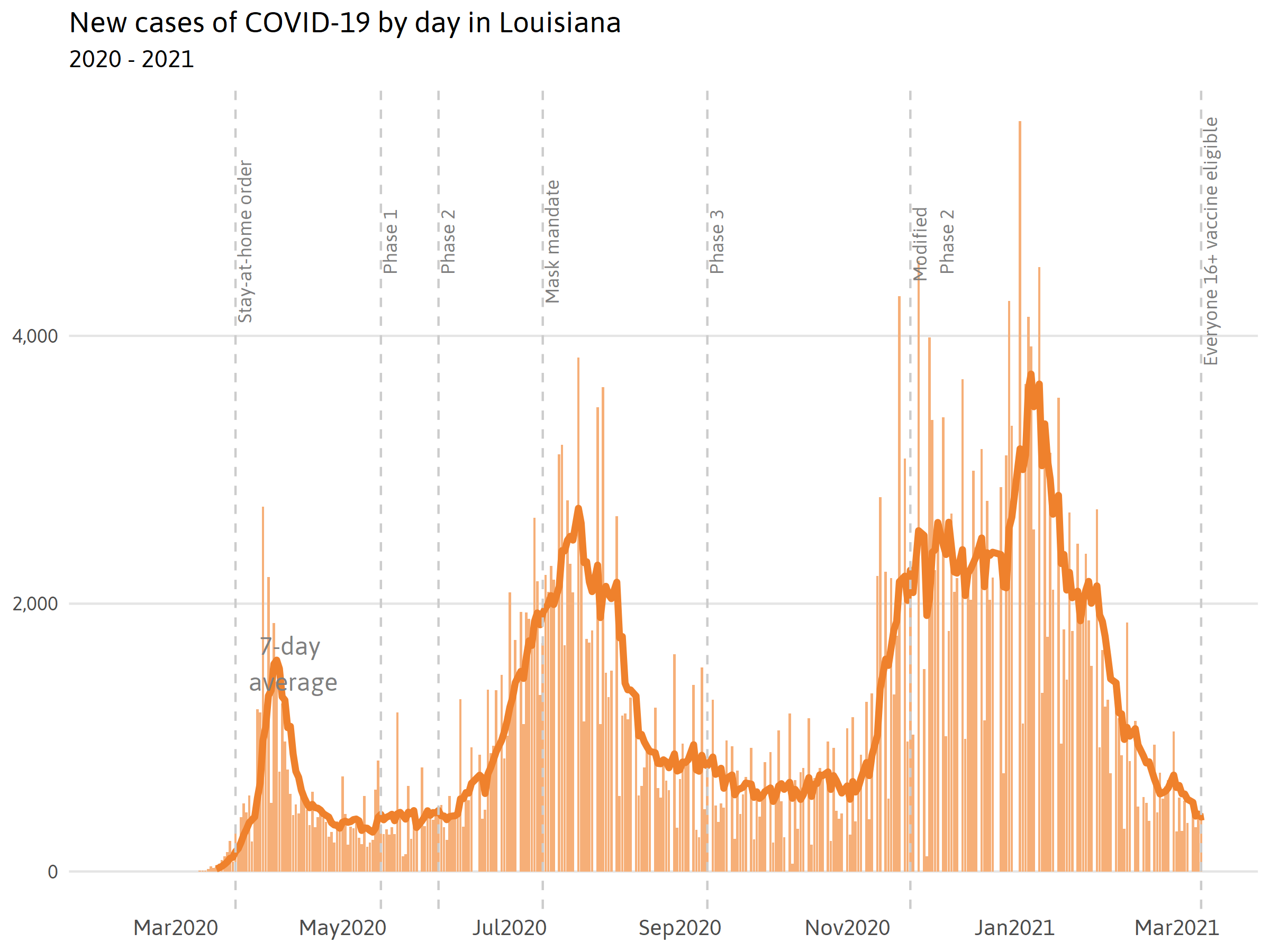
COVID-19 (Novel Coronavirus) is a highly contagious and deadly disease with few treatment options and no vaccine. The first presumptive positive case of COVID-19 in Louisiana was reported on March 9, 2020 and quickly spread across the state thereafter. By April 11th, every parish in Louisiana had at least one reported case. Several of the first individuals diagnosed with COVID-19 in Louisiana had not traveled abroad nor been in close contact with a known case, which indicates that there is widespread community transmission of COVID-19 beyond what is being captured in the data at this time.i
Confirmed cases and deaths in Louisiana over last 10 days
To be clear, the number of reported confirmed cases in Louisiana is not solely a reflection of the number of people becoming infected, but also reflects changing testing accessibility and capacity.ii
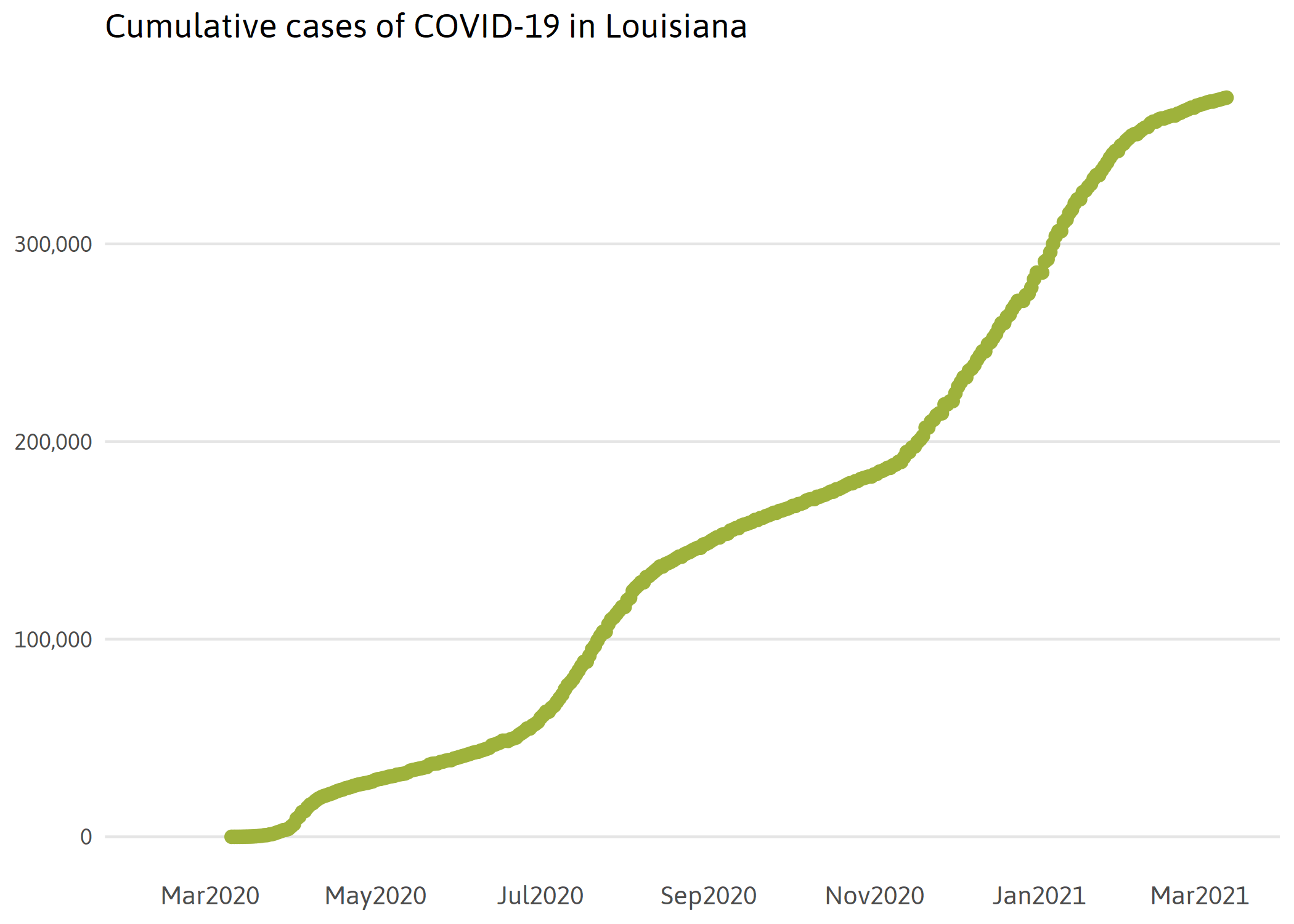
Initially, most cases in Louisiana were confirmed by the Louisiana Department of Health laboratory. Commercial testing in Louisiana began to ramp up on March 19th, expanding testing capacity in the state exponentially. At first, only drive-through was available for health care workers and first responders in New Orleans.iii On March 22nd, limited testing became available to those with severe symptoms of COVID-19.iv By late April, free neighborhood walk-up testing improved accessibility to those who do not have a car. As COVID-19 spread to the rest of the state, federally supported drive-thru testing sites in Baton Rouge expanded capacity immensely. Testing is now available at many clinics and health care facilities across the state. However, due to bottlenecks in processing, wait times for results still vary significantly, reducing the usefulness of the test.
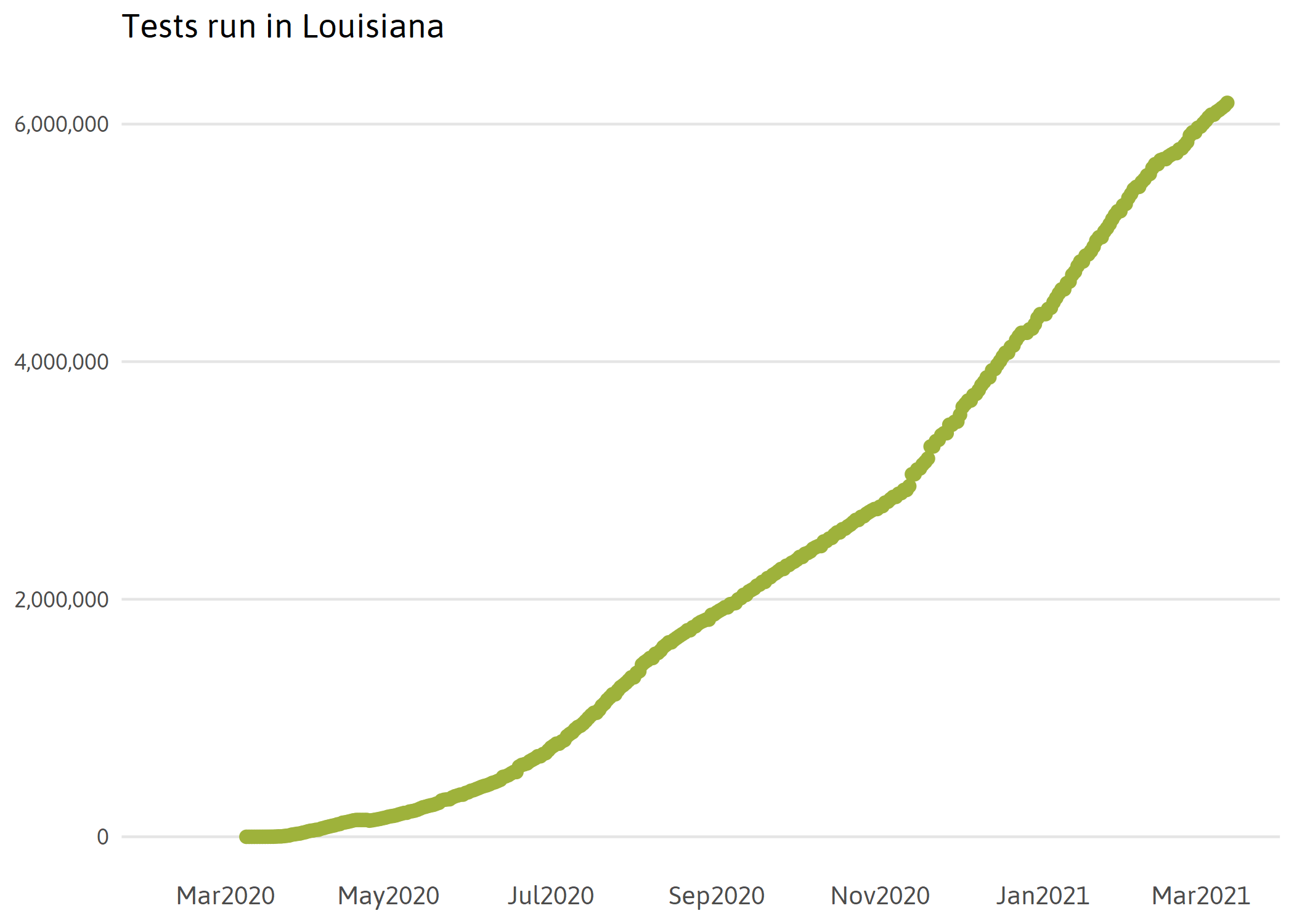
Note: The Louisiana Department of Health is conducting a comprehensive review of commercial testing numbers. These data will be updated upon completion of this review. This does not impact the number of positive cases reported. Positive cases are updated and accurate.
In Louisiana, people of all age groups have tested positive for COVID-19. While children can contract COVID-19, they are at a much lower risk of becoming severely ill. Asymptomatic children are much less likely to seek testing, but can still infect others.v The elderly and those with pre-existing conditions are at a significantly higher risk of fatality. In Louisiana, most people who have died by COVID-19 were over 70 years of age. Therefore, to protect our most vulnerable neighbors, it is vital for all people to follow self-isolation guidelines regardless of age, health status, or individual risk.
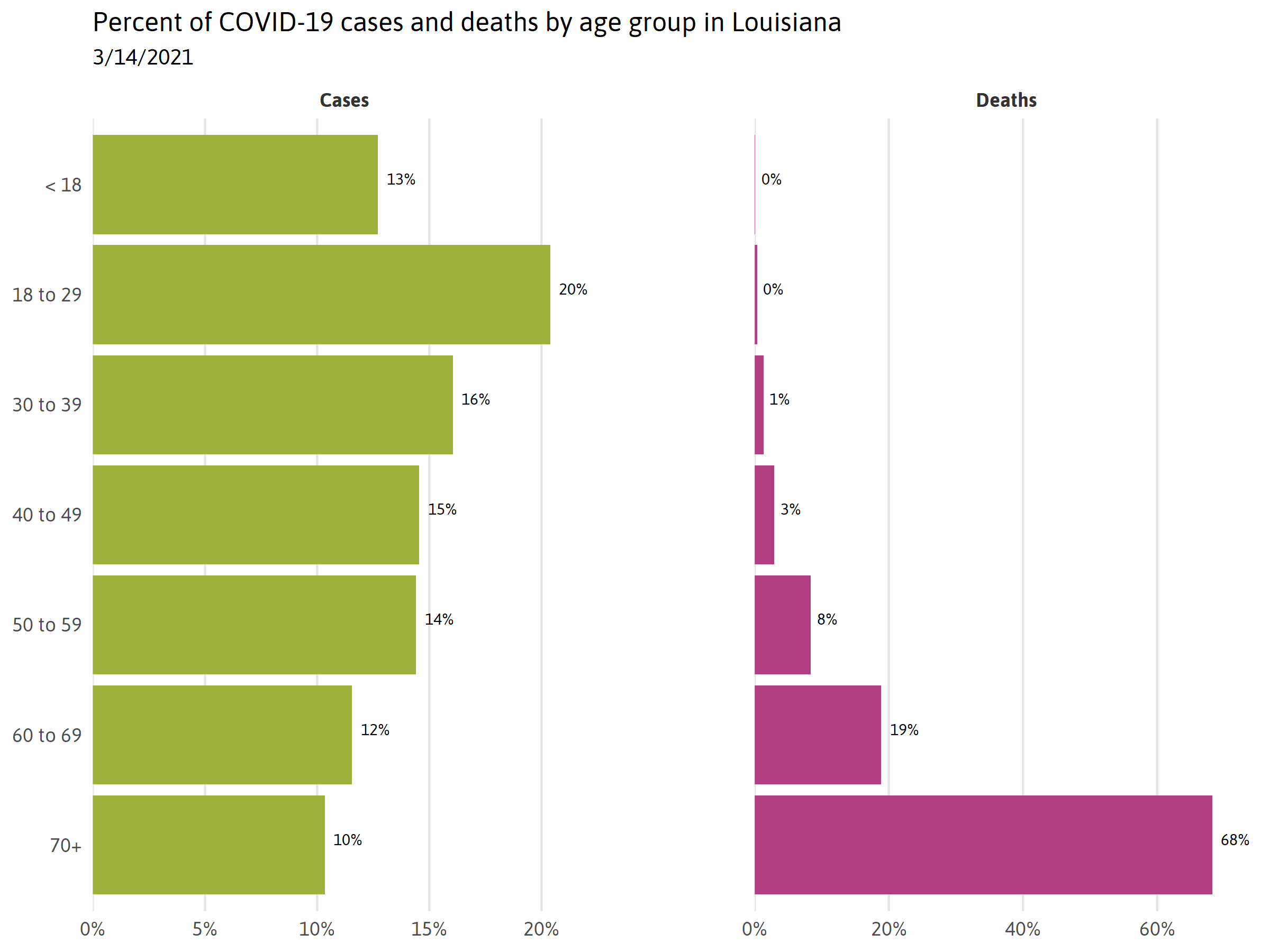
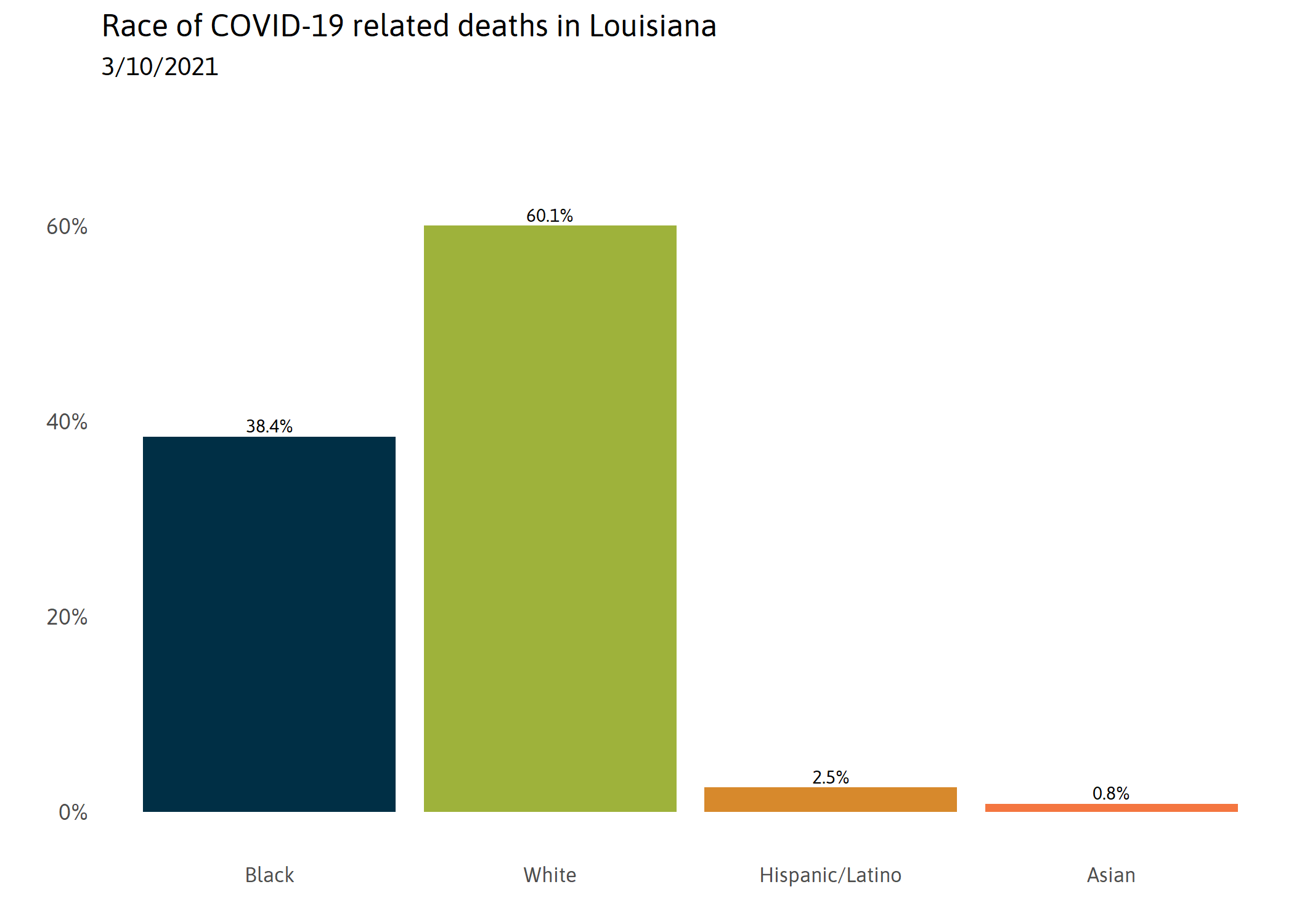
Black Louisianans are dying of COVID-19 at a disproportionately high rate in Louisiana.
The true magnitude of the disparity in COVID-19 deaths by race is apparent when interpreted alongside state demographics. Only 32 percent of Louisiana’s population is black, while 58 percent is white. Among adults over 65 years of age, the riskiest age group for COVID-19 fatalities, only 25 percent of Louisiana’s population over 65 is black, compared to 70 percent white.
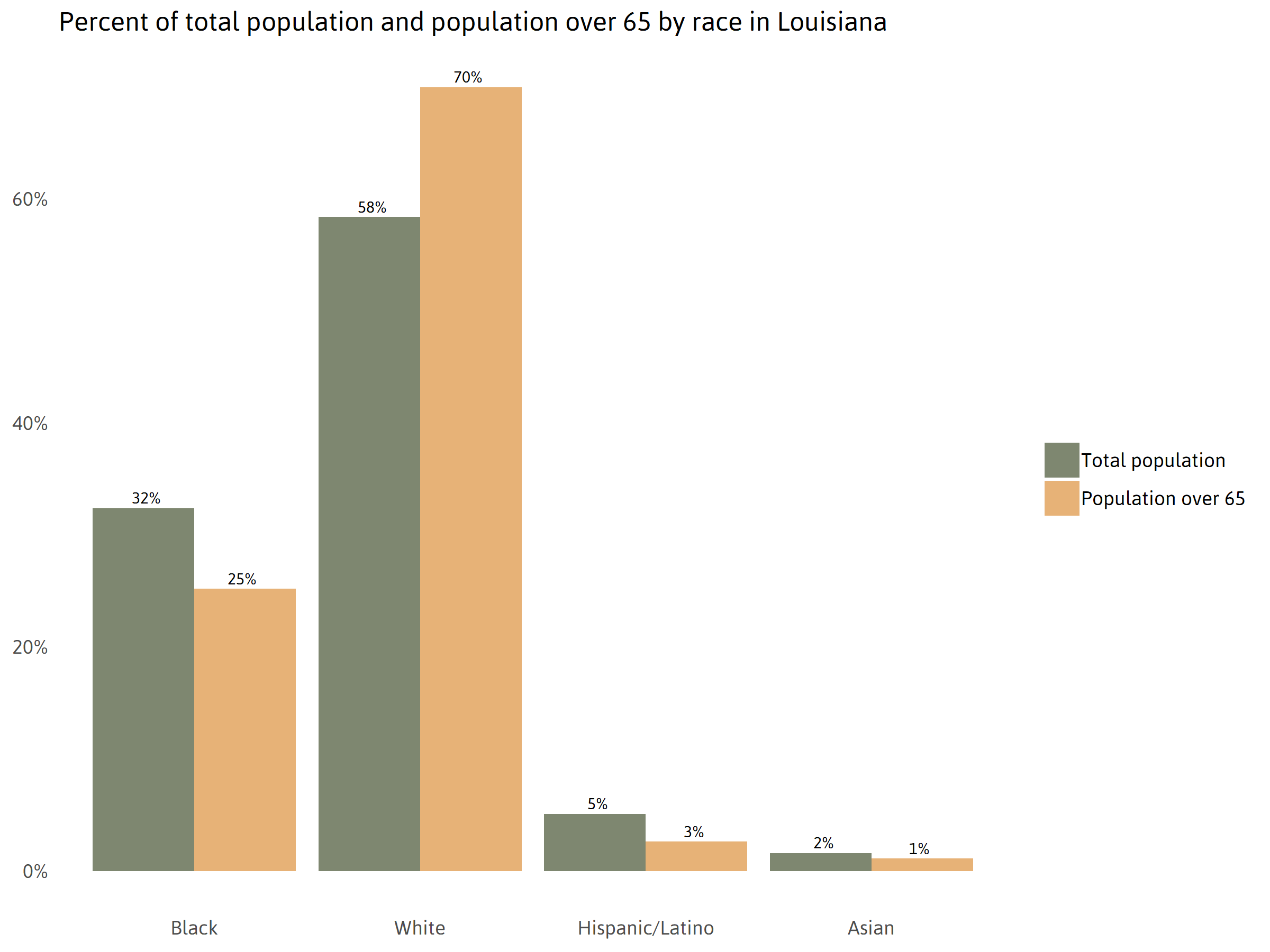
Note: “White” refers to individuals who report to be only one race and not Hispanic. “Hispanics” can be of any race(s).
Emerging studies have linked conditions such as hypertension, diabetes, and kidney disease to higher risk of fatal COVID-19 complications.vi Initial data reported that high blood pressure was the most common comorbidity present at time of COVID-19 related death in Louisiana. To be clear, that does not mean that having high blood pressure puts you at highest risk. In 2018, 68 percent of Louisiana’s population 65 years and older had been diagnosed with high blood pressure.vii
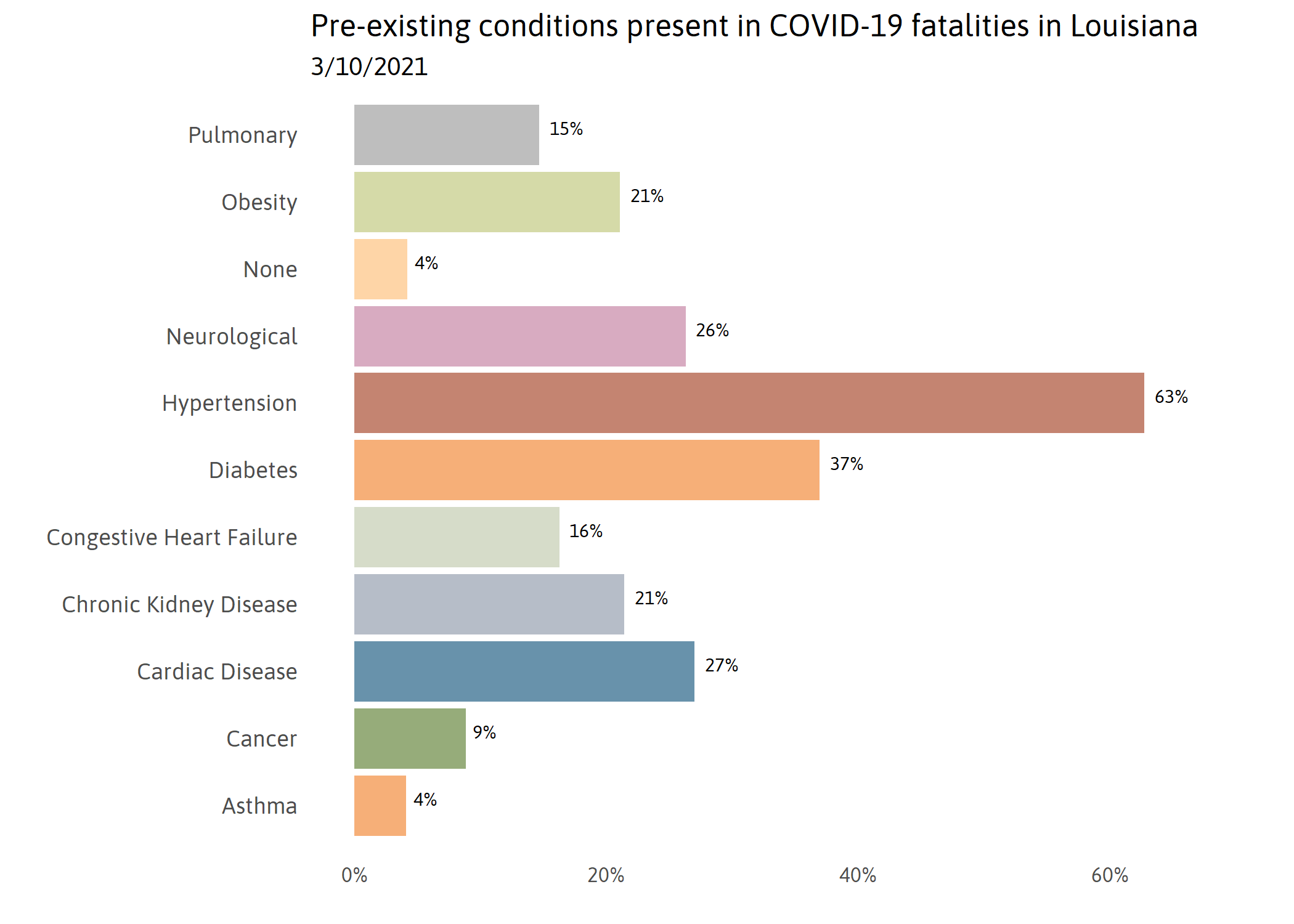
More data is needed to clarify the relationship between pre-existing conditions and fatal COVID-19 outcomes. However, initial data makes it clear that racial disparities in pre-existing conditions alone does not explain the disproportionate number of black Louisianans who have died from COVID-19.
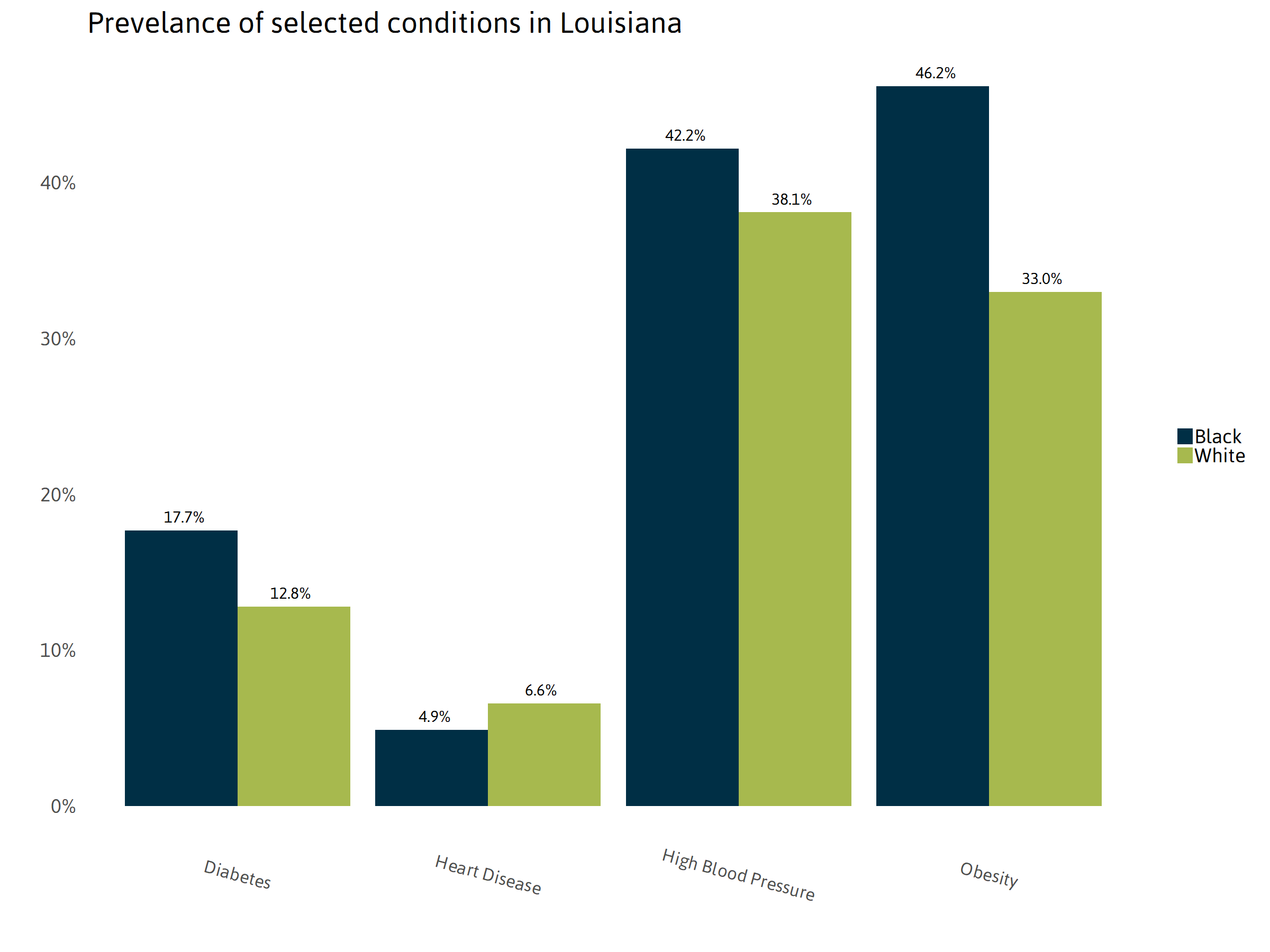
There is still much to learn about what makes a region more susceptible to COVID-19. Regardless, it is clear that COVID-19 quickly found a foothold in Louisiana and has since spread rapidly. From the first reported case, it only took one month to reach every parish in the state.
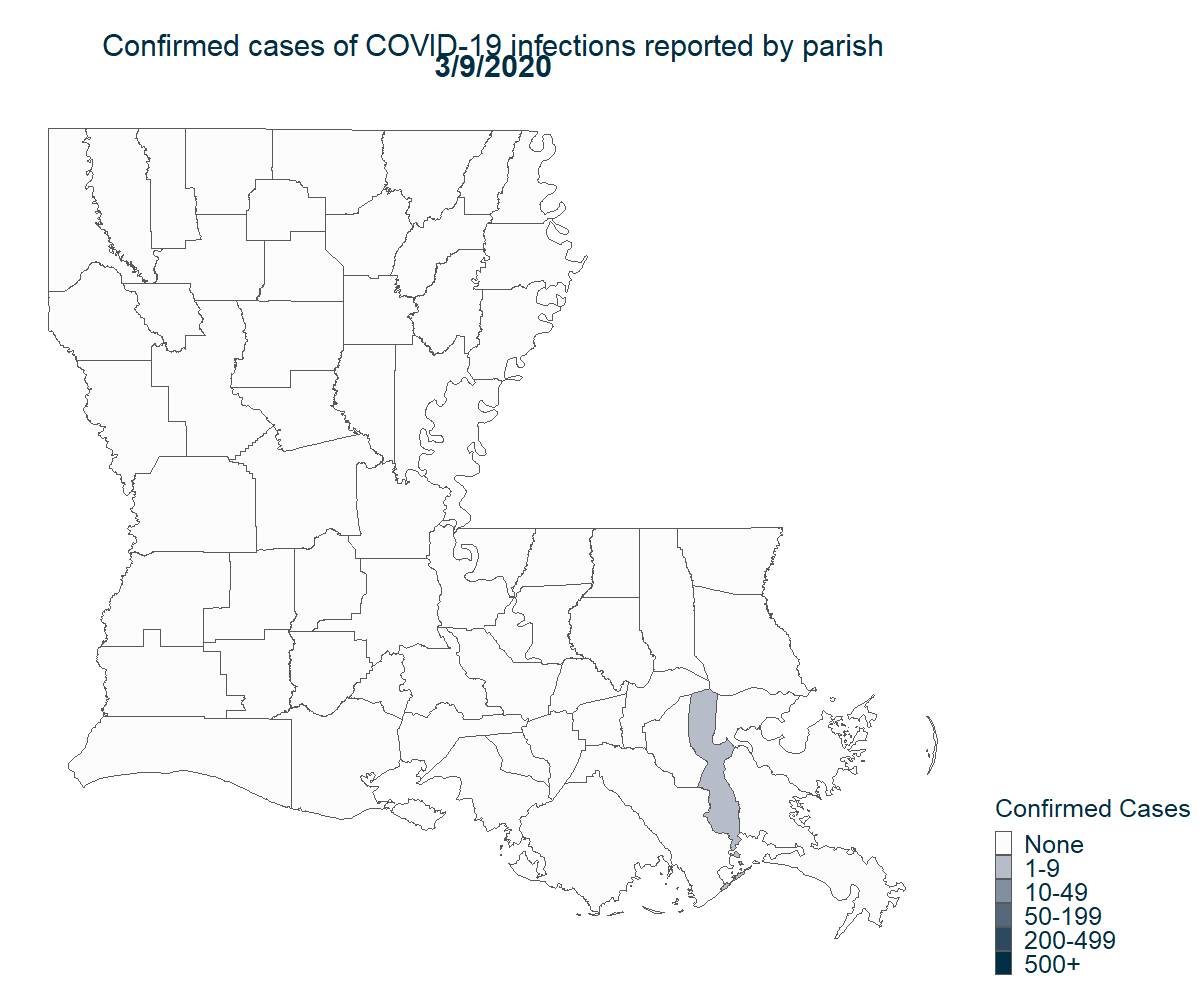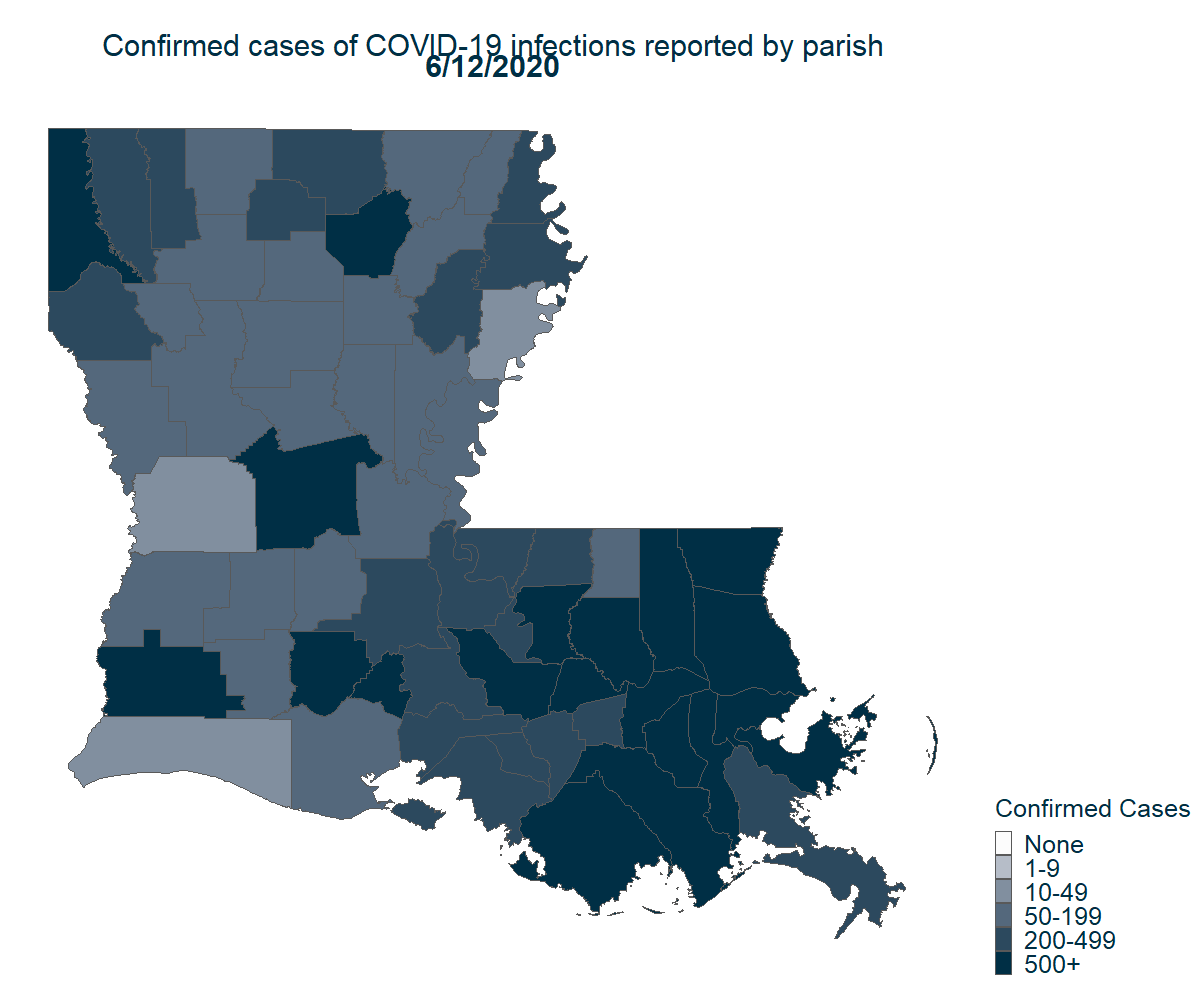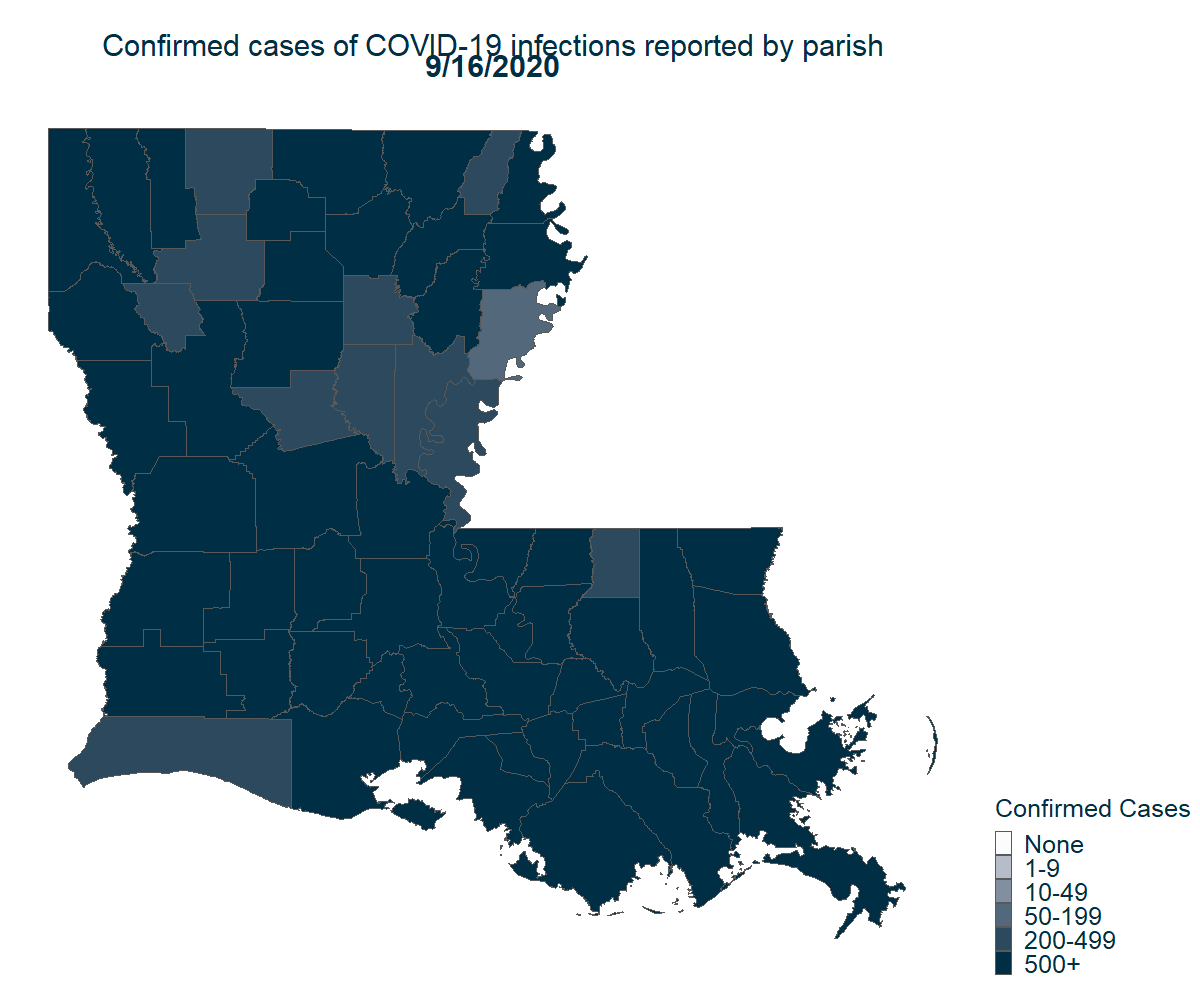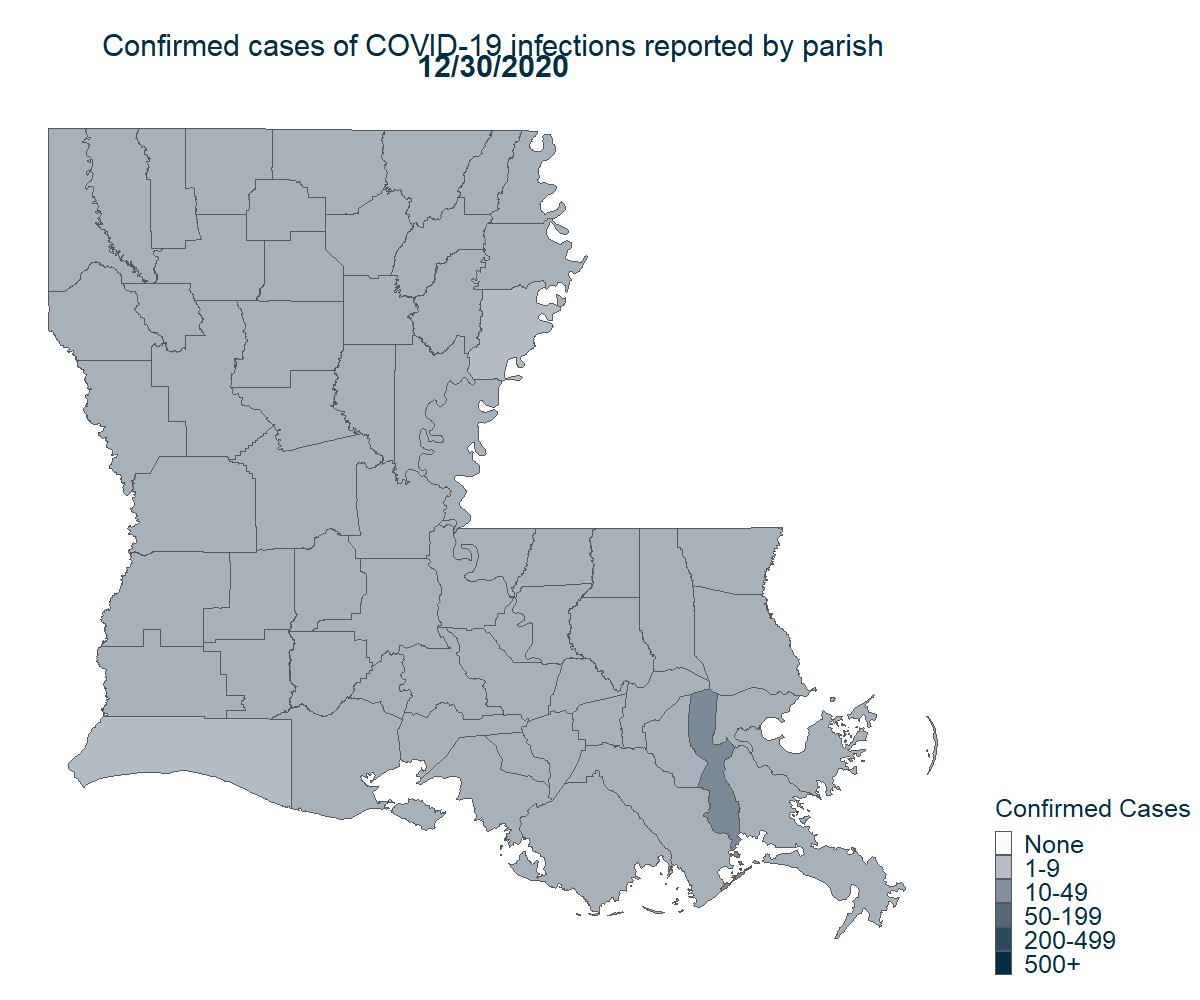
Note: Cases are assigned to a person’s parish of residence regardless of where they seek care.
While Orleans Parish was initially the epicenter of the state’s outbreak, COVID is now present in every parish in Louisiana. Early on, St. John the Baptist Parish’s high infection and death rate gained national attention. On April 10th, St. John had one-sixth the number of deaths as Orleans Parish but one-and-a-half times the rate of deaths per 100,000 residents. This is because the population of St. John parish is much smaller, so the number COVID-19 cases proportional to the population ranked amongst the highest in the country. As of June 15th, nearly half of the deaths in St. John were attributable to outbreaks in two nursing homes.
Confirmed cases in parishes with most cases in the state
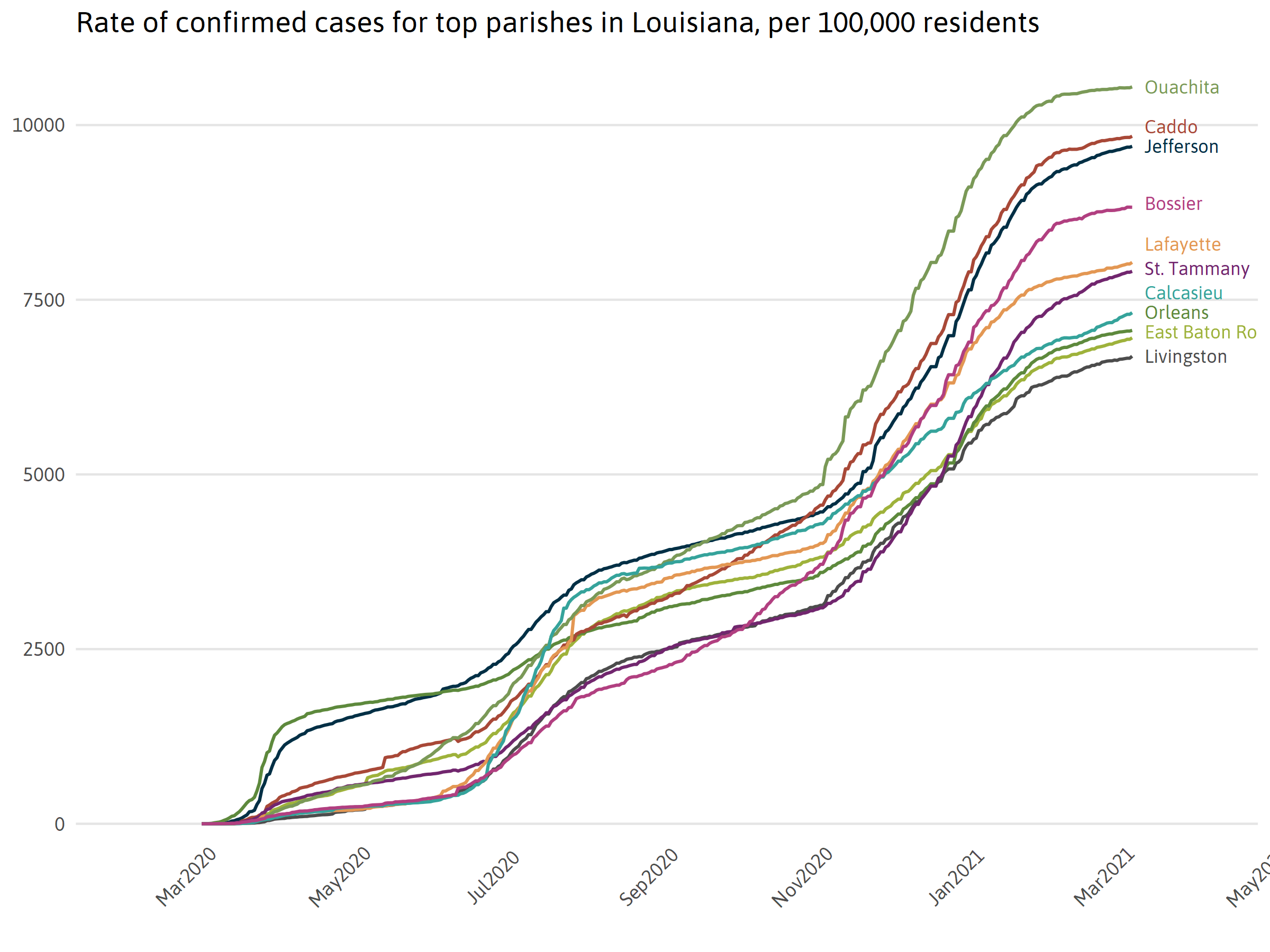
Confirmed deaths in parishes with most cases in the state
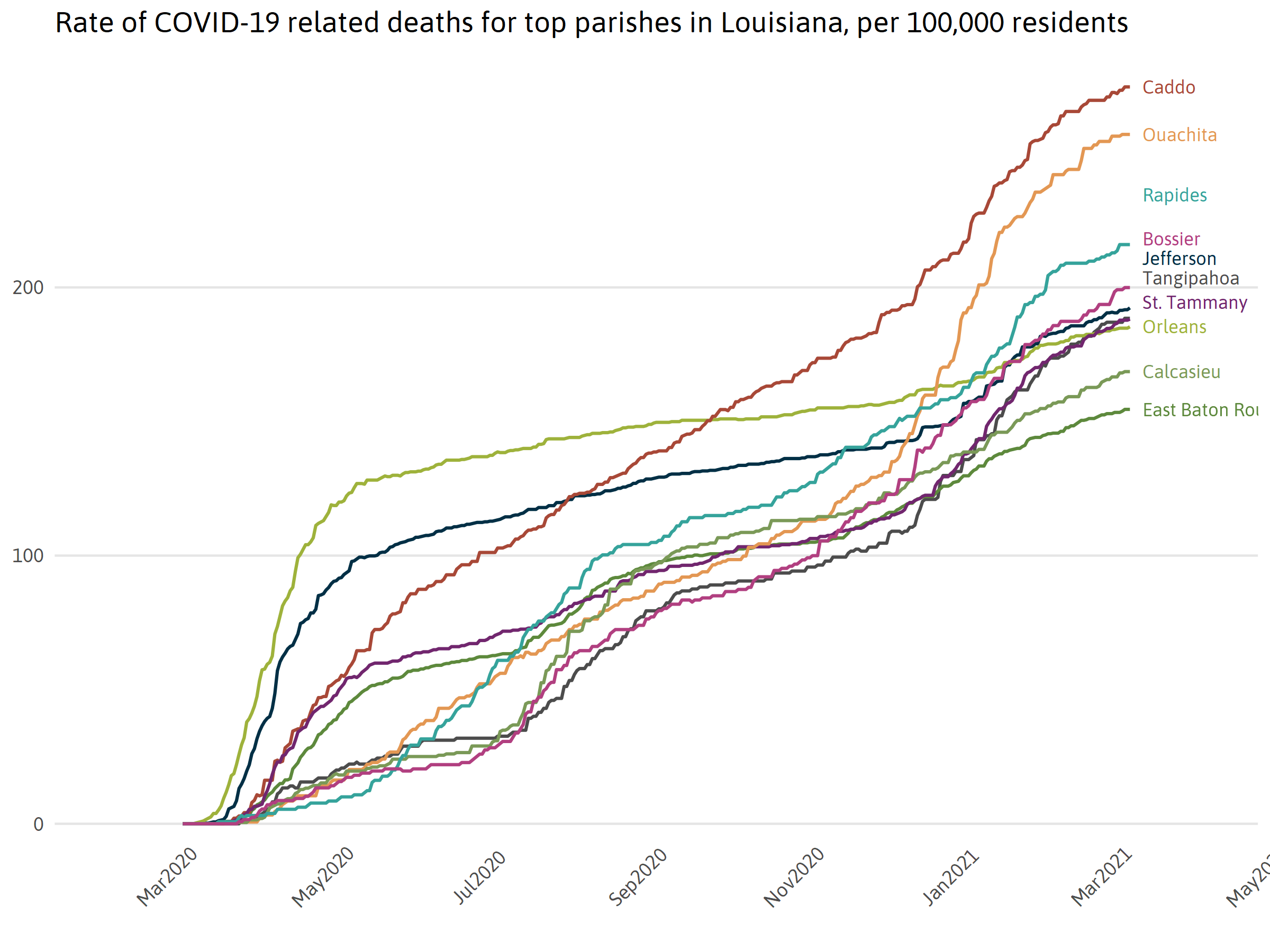
Comparing COVID-19 in top parishes to other hot spots in nation
Examining the rate of COVID-19 infections per population can be used to compare the impact across regions with different population sizes.
Unlike the number of confirmed cases, which can be affected by the number of tests administered and the various waiting periods for test results, the number of deaths in a region is less influenced by testing decisions. Death rates reflect a combination of the true infection rate, available health care resources, and local demographic characteristics.
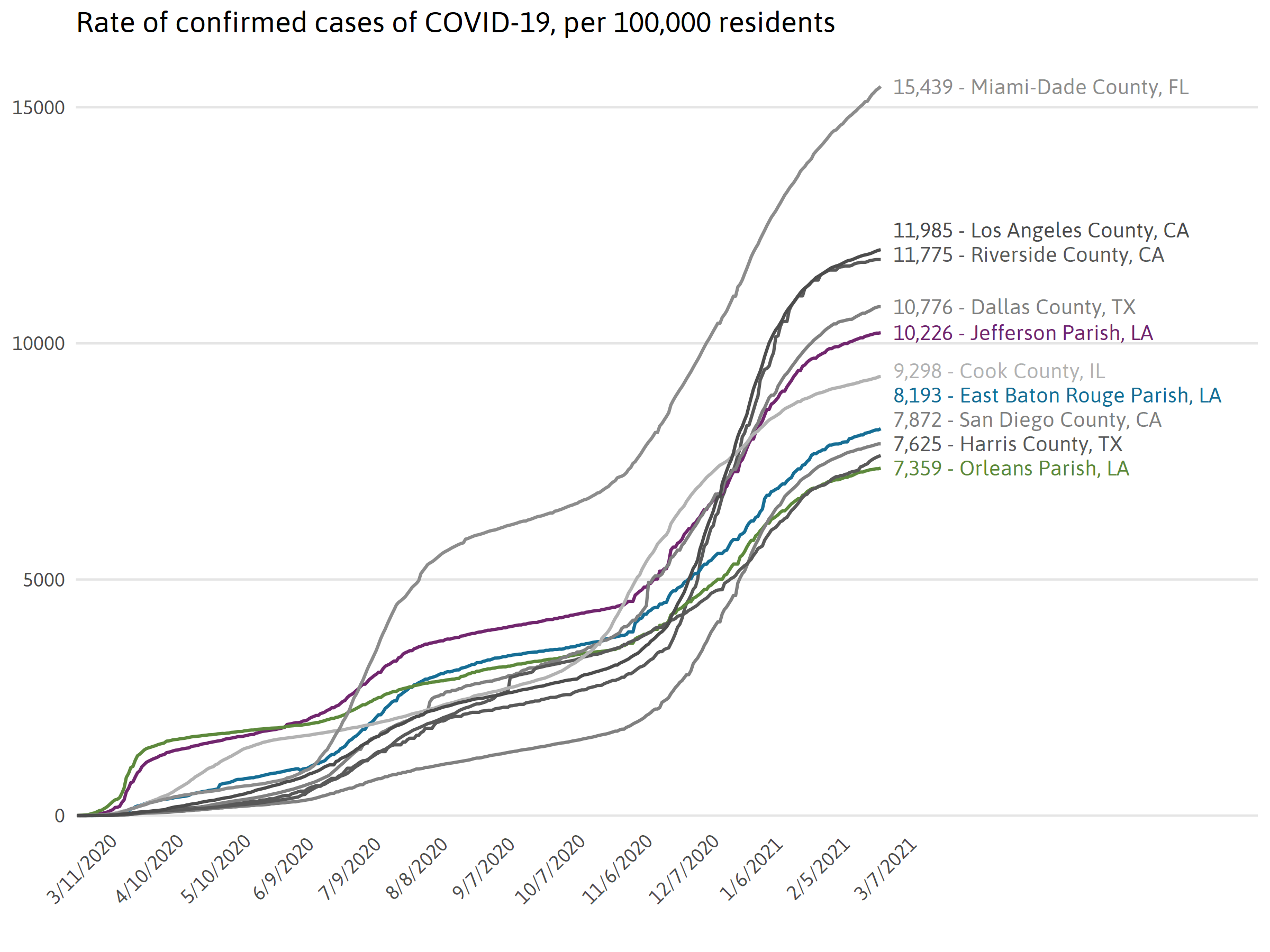
Note: The three parishes in Louisiana included have the highest number of cases on the latest day data was available. The list of comparison counties is comprised of the top seven counties in the U.S. with the largest total number of cases on the latest day data was available. New York City, NY is the 5 boroughs of New York City. Though data is available on the individual boroughs, the State of New York has most commonly chosen to report it in aggregate as New York City.
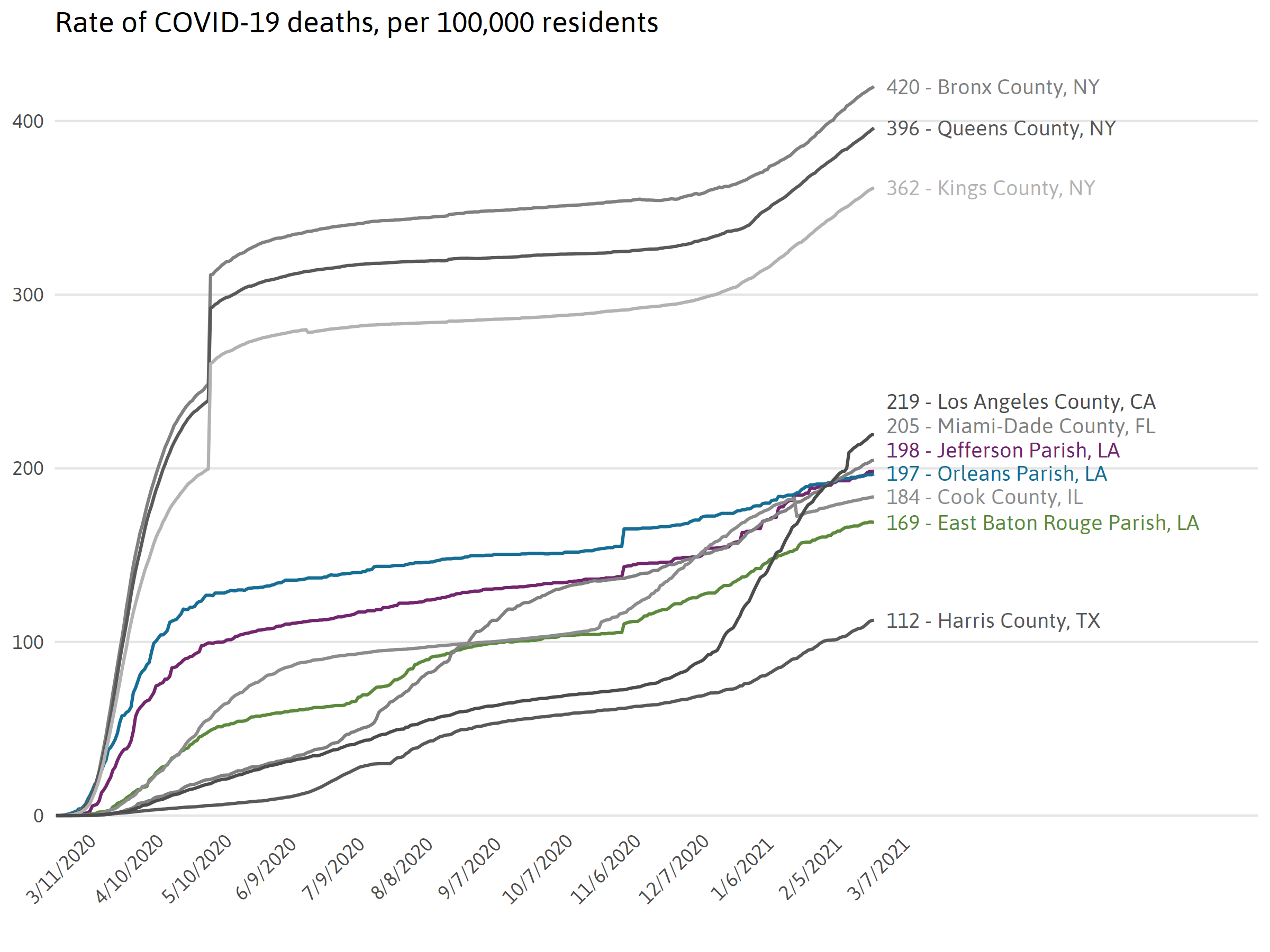
Note: The list of comparison counties are comprised of the top 10 counties in the US with the largest total number of deaths on the latest day data was available.
Cases and deaths in New Orleans
The first case of COVID-19 in Louisiana was in Orleans Parish. Soon after, New Orleans led the metro, state and much of the nation in the number of confirmed cases. Orleans Parish has since been outpaced by many other parishes.
Confirmed cases and deaths in New Orleans over last 10 days
The first COVID-19-related death in Orleans Parish happened on March 14th, 2020, and by March 26th, COVID-19 had killed more New Orleanians than the flu and pneumonia did in all of 2018. In fact, within only three weeks, it had killed more residents than several of New Orleans’s leading causes of death do in an entire year, including accidental drug overdose, homicide, and Alzheimer’s disease.
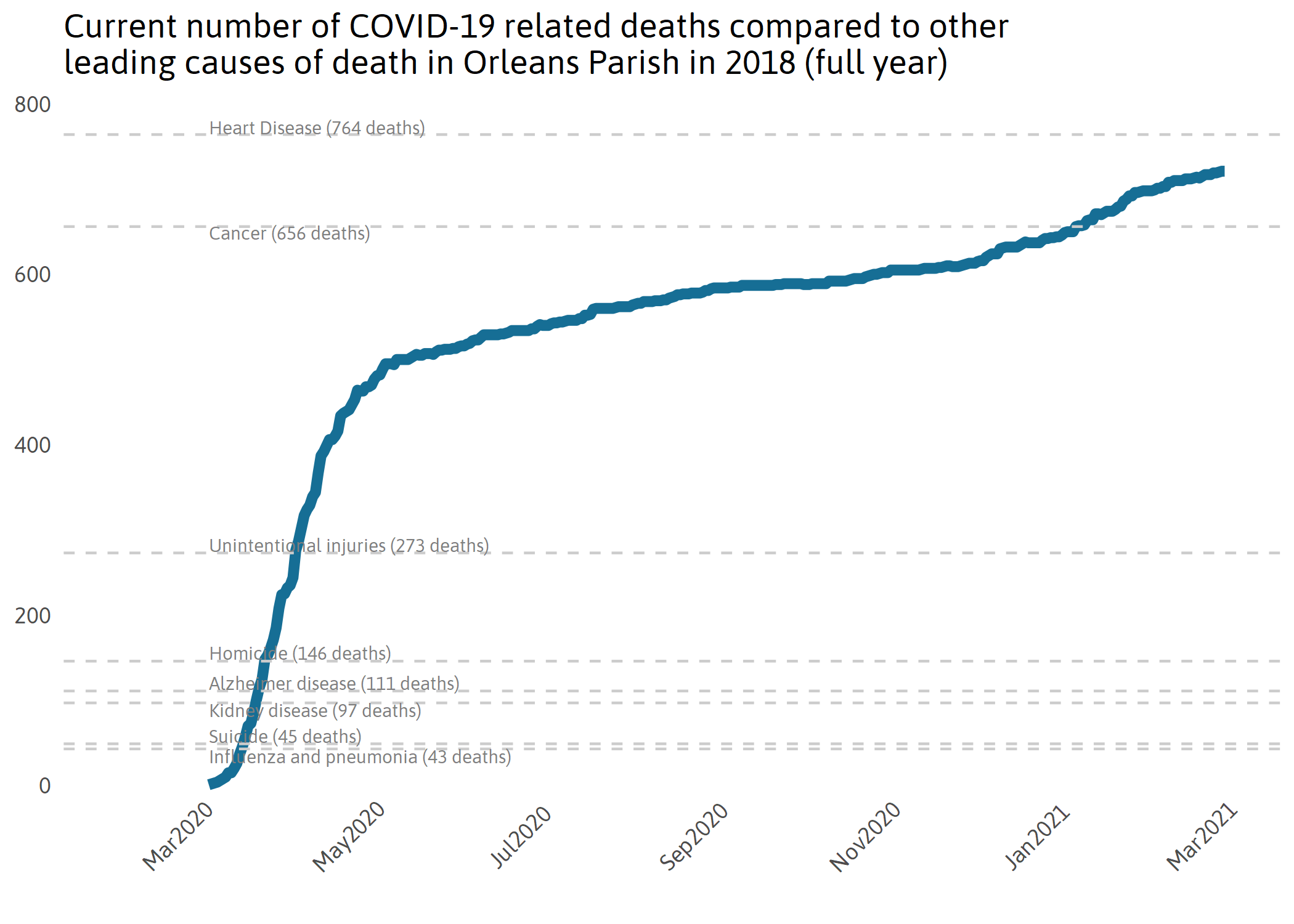
Note: All 2018 cause of death data comes from CDC Wonder except for homicide which comes from FBI UCR.
Cases and deaths in New Orleans metro
The first cases of COVID-19 in Louisiana were in New Orleans metro. Orleans and Jefferson Parish still have the highest number of cases and deaths in the region.
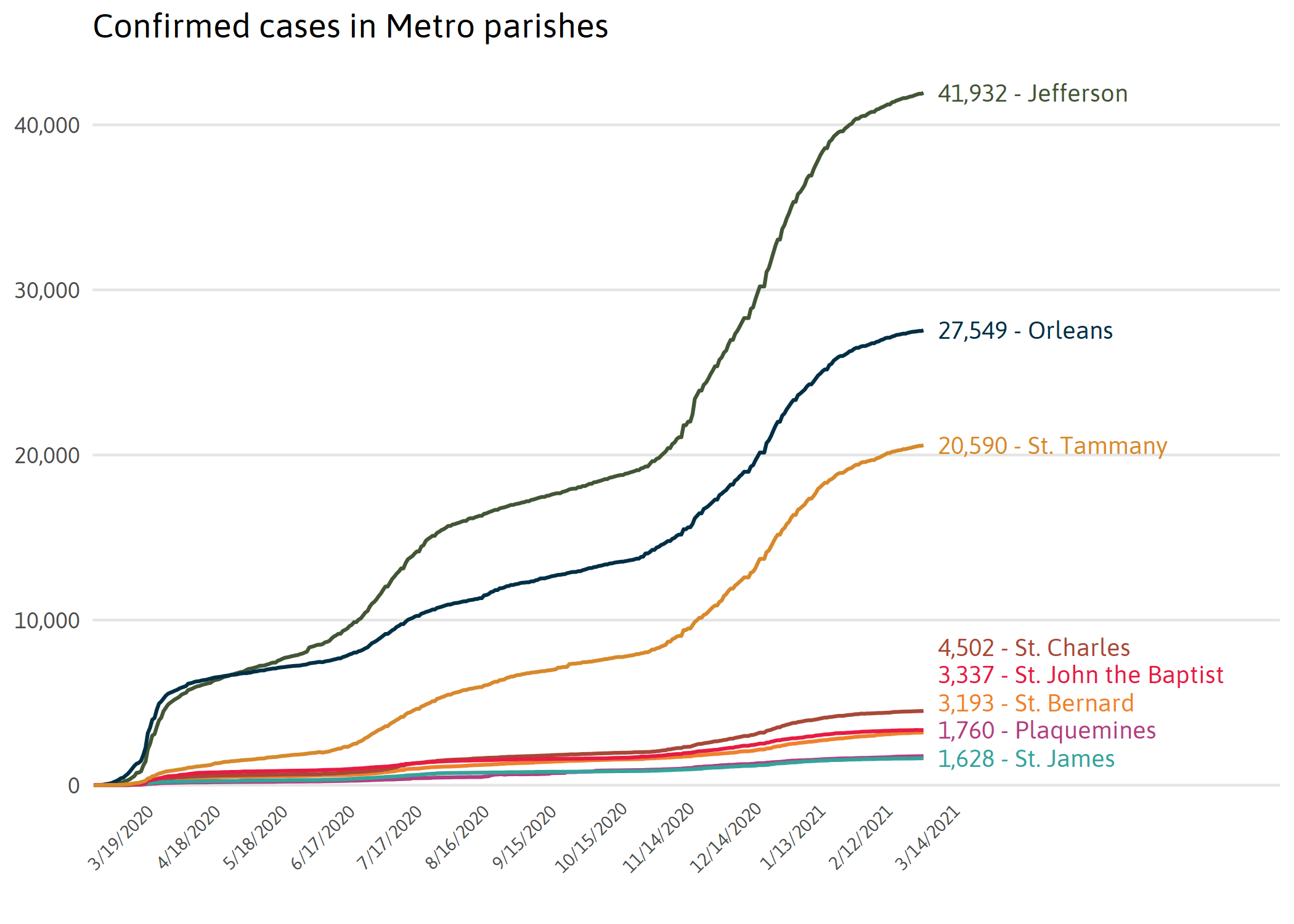
Note: Cases and deaths are assigned to a person’s parish of residence regardless of where they seek care.
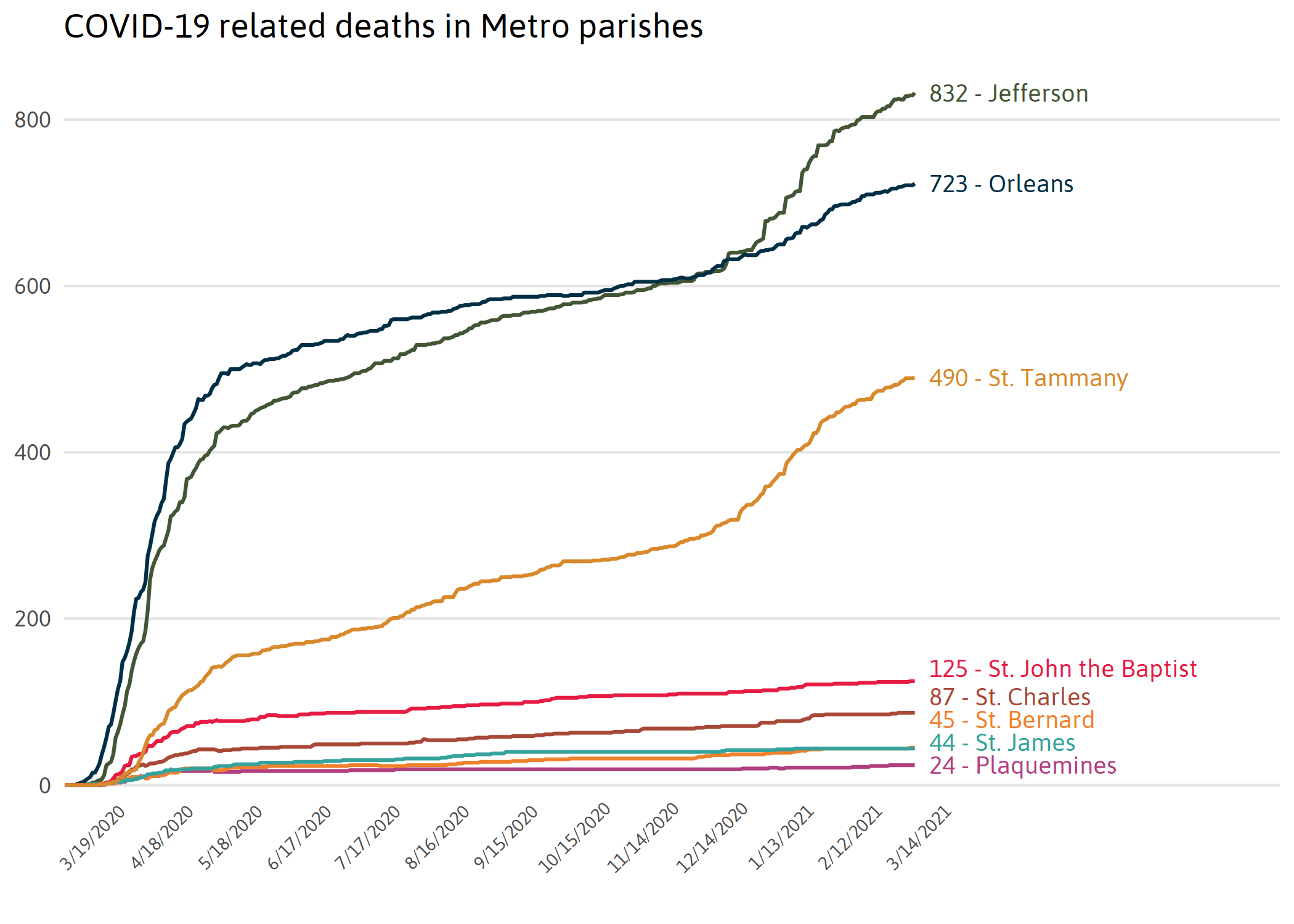
Note: Cases and deaths are assigned to a person’s parish of residence regardless of where they seek care.
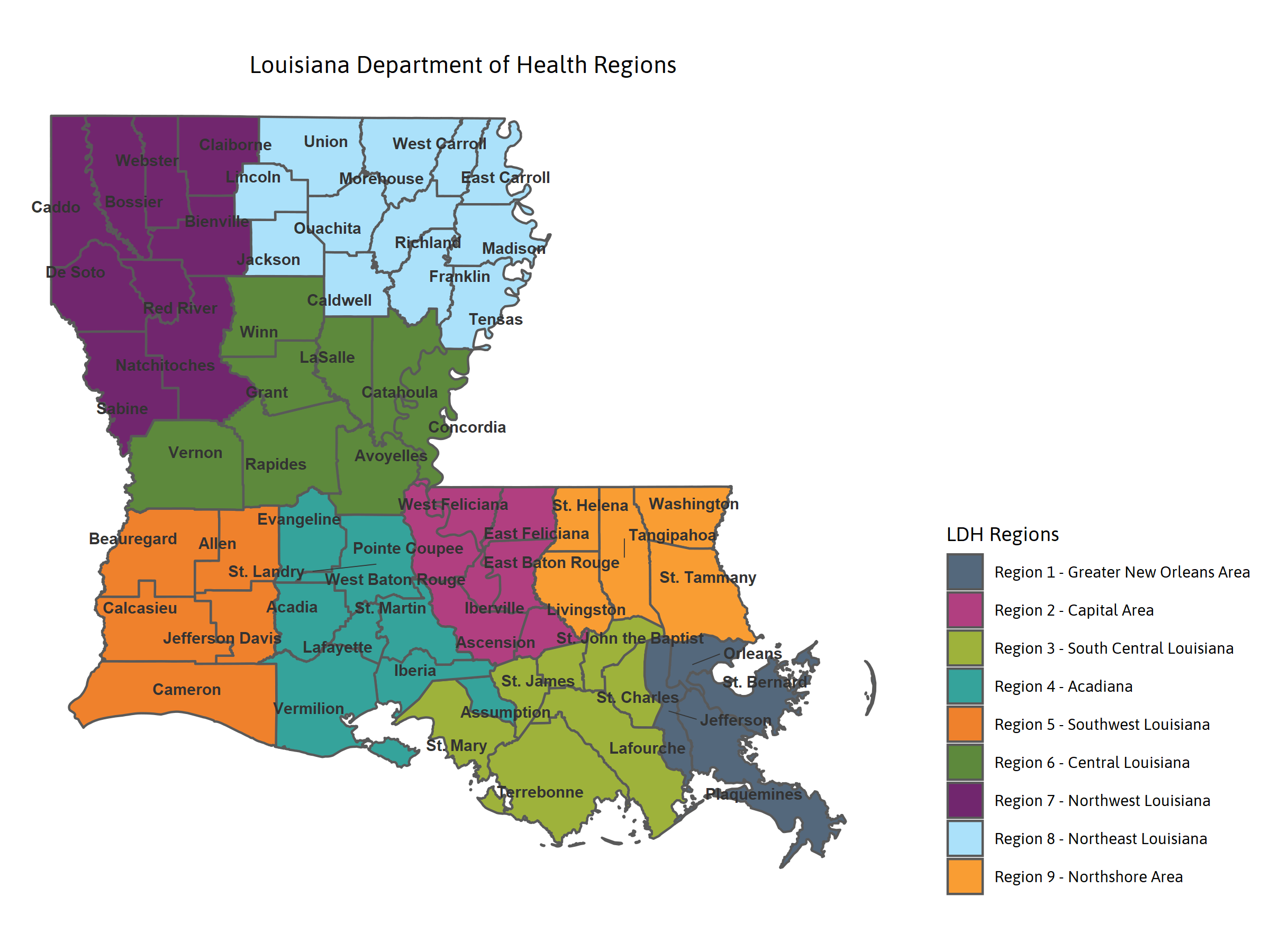
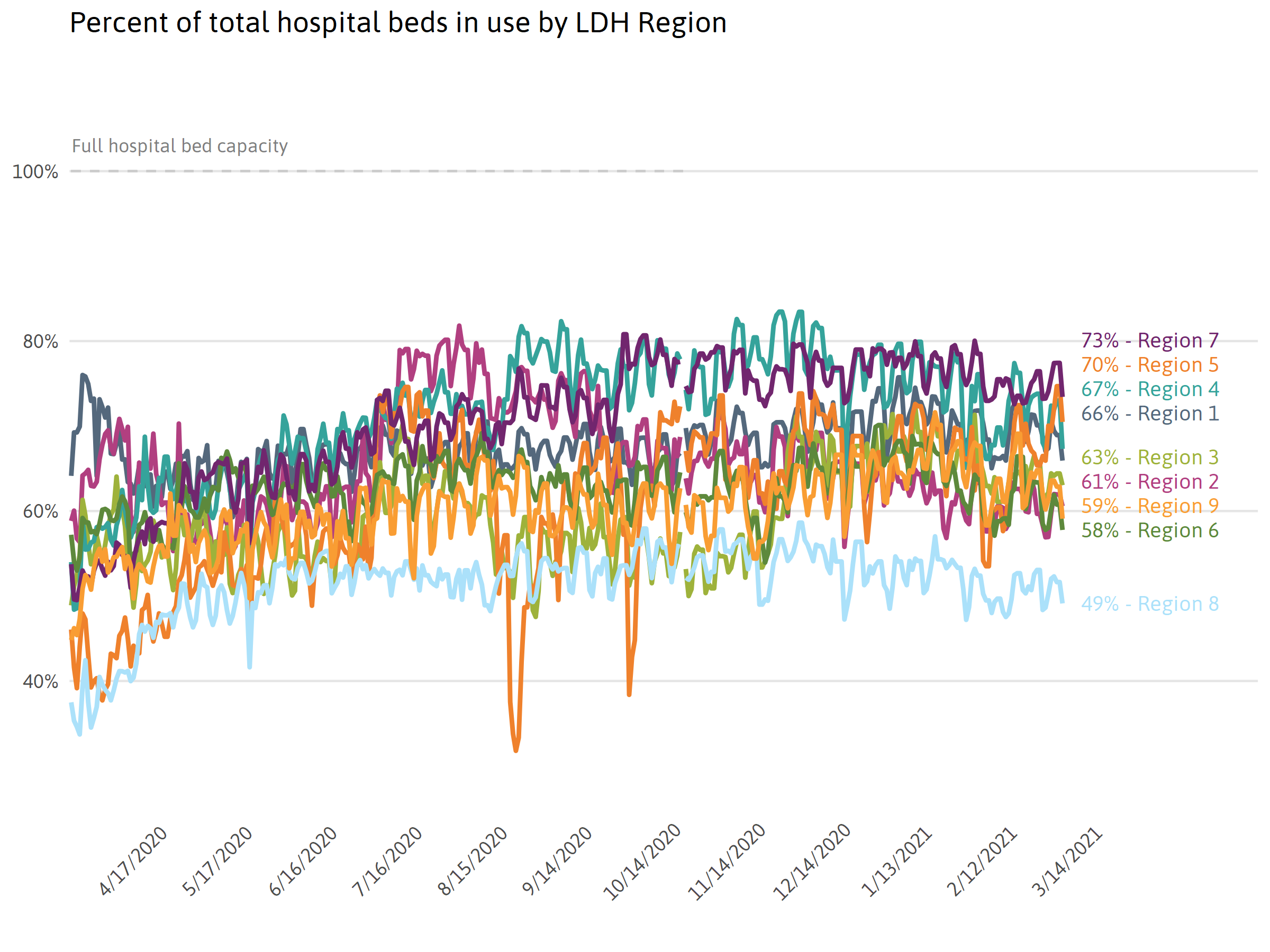
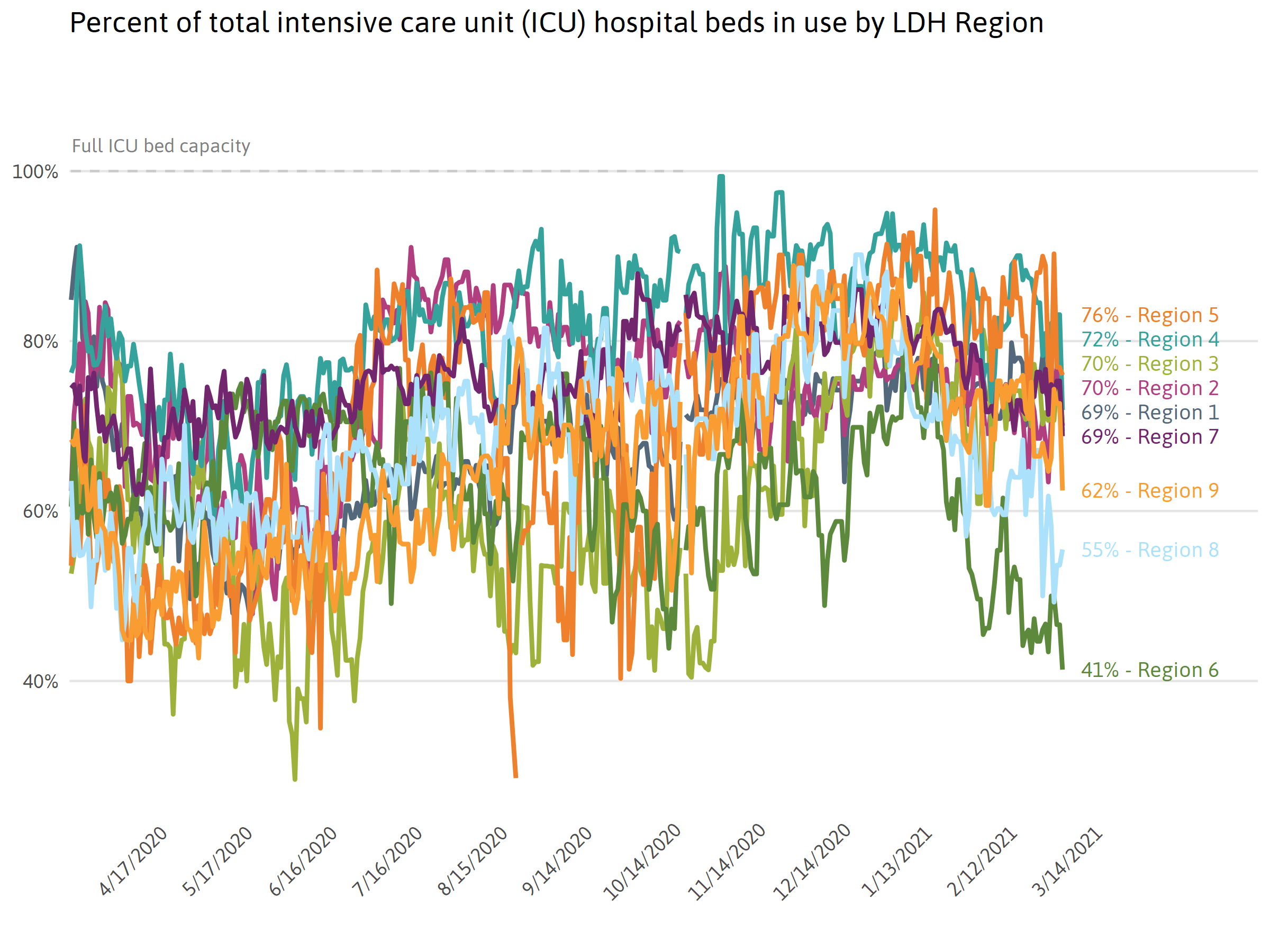
Tracking health care resources across Louisiana
In late March, Governor John Bel Edwards announced “worst-case scenario” predictions estimated that health care resources in several regions of Louisiana could be overwhelmed by early April, leaving the health care system unable to treat hundreds.viii In terms of ICU beds and ventilators, the number of patients unable to be served could die without critical care. Under “best-case scenario” predictions, Louisianans would have to act quickly to reduce the spread of COVID-19 by adhering to strict social-distancing guidelines.ix Monitoring resource usage relative to overall capacity is critical for regional planning. The graphics below depict how much of these three health care resources are currently in use. Fluctuations may be a result of the actual number of resources being used, newly acquired resources, or the movement of non-COVID-19 patients to free up space.